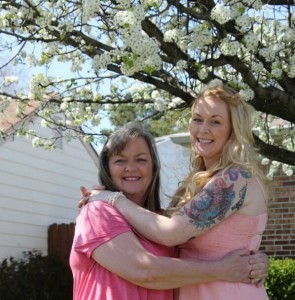 Self management of my Type 2 diabetes
Self management of my Type 2 diabetes
First year to March 2017
Thousands of people suffering from erratic blood sugar has been using this ground-breaking solution…
To help them burn away dangerous fat from their vital organs and bellies…
While stabilizing their blood sugar levels naturally and effectively.
And starting today…
Summary
- Diagnosed Type 2, February 2016 (HbA1C 66 mmol/mol, 8.2%)
- Low-carb diet
- Self-testing
- No medication
- Now in non-diabetic range (HbA1c 37 mmol/mol, 5.7%)
- 22 kg weight loss
- Improved lipid profile
My introduction and diagnosis
My first blood test was in February 2016 following reported exhaustion and listlessness. There were none of some ‘classic’ Type 2 sysmtoms of excessive thirst, blurred vision, need to urinate etc.
I remember that the diagnosis was confirmed on 23 February with an HbA1c of 66 mmol/mol (8.2%). It later transpired that in 2010 I had an HbA1c of 45 (6.3%) on a blood test.
No guidance was given, but I was told that this was life-changing, just to lose weight (I was 92 kg, BMI of 32.6), and exercise more and make an appointment to see my diabetes doctor. The earliest appointment available was for 18 March, over four weeks away. Considering elevated blood pressure (the spot reading of 162/92 while blood sample taken) then I was told to take three weeks of reading to make this appointment (where? How? – buy myself a meter or at a chemist, good, thanks)
As a result of total cholesterol of 7.0 I was prescribed Simvastatin (I never took this) without my prior agreement and any explanatory discussion.
Something about me
Actually I have never been one of taking medication if I will help it. Our human body is always underestimated as a great self-healing mechanism. Some paracetamol per year is usually more than enough for me. It is important.
I’m a scientist by training and when faced with something like this then my first reaction is to find out about it plus not take anything at face value without assessing it personally.
On the other hand my Type 2 diagnosis was a wakeup call and the kick I had to sort my weight as well as well being out. I immediately started walking for around 50 minutes daily (average).
I studied on the internet and found a diabetes treatment video; learned about carbs and the impact on blood sugars levels; could understand the logic of LCHF diets; plus just went for it at 50 g carbohydrates daily –no pasta, no rice, no potatoes, no bread. Thankfully I didn’t have the withdrawal symptoms often experienced by altering so abruptly. And I purchased a blood glucose monitor in the mall and started testing myself. Happily I started losing weight straight away since I got into ketosis plus my body started to burn preferentially burn stored fat for energy. That’s good.
I also read about statins and cholesterol and decided that I was not going to touch all of them with a barge pole. I do it myself.
First DN appointment
Four weeks in and I was already making progress on exercise and diet alone.
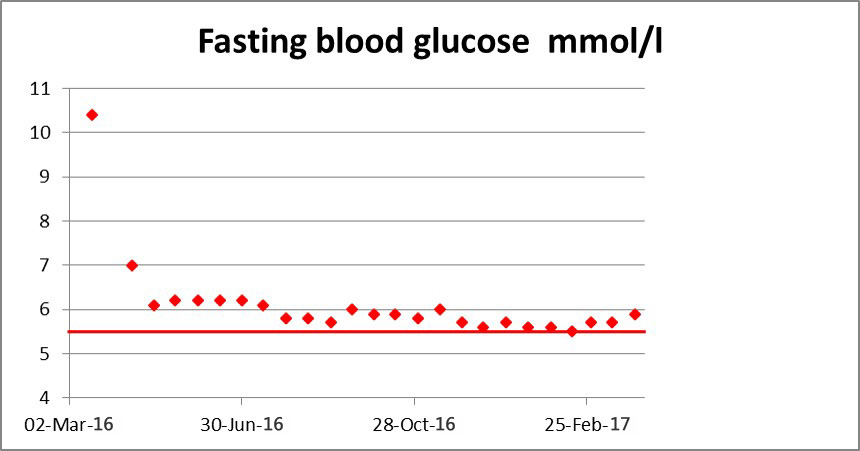
Fasting BGs were down from over 11 mmol/l to about 6.6; pre-dinner BGs in the high 5s; plus BGs 2 hour after eating in the mid 7s and high 6s, hence I was understanding what I couldn’t and could have in terms of my blood sugar management.
My weigh went down from 95 kg to 86.8 kg, and my blood pressure was down to about 140/80.
I know it was agreed for me to carry on with exercise and diet myself without medication, with a review in four months times.
Interim progress
In august 2016 my HbA1c was down from 60 to 45 (6.3%), so that I was in the prediabetic range now.
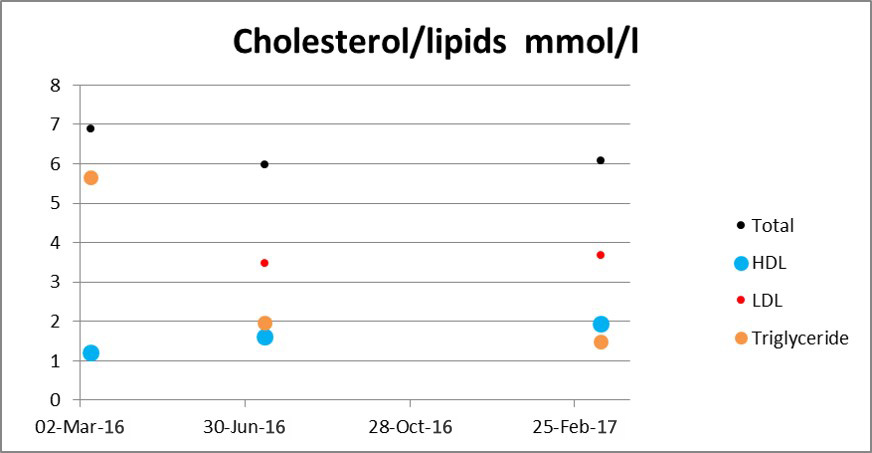
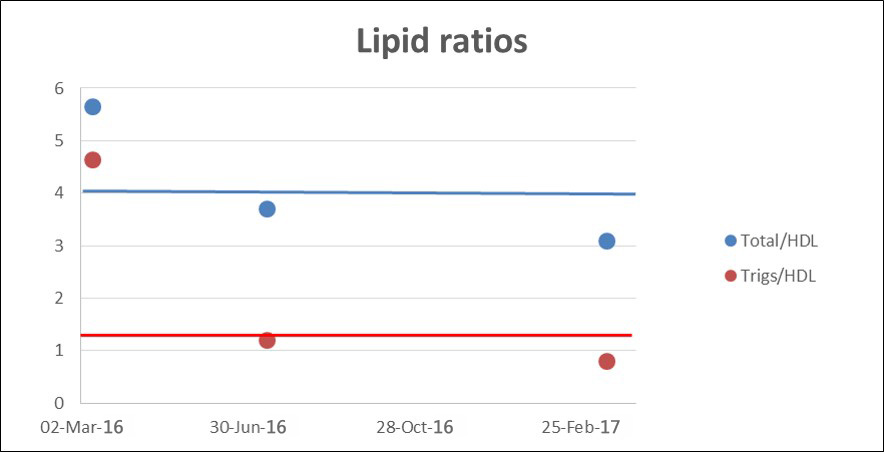
Total cholesterol was down to 6.0, however more importantly the triglycerides were down from 5.67 to 1.98 mmol/l, plus HDC-C was up from 1.23 to 1.63, with triglycerides/HDL and total/HDL ratios both dropping into the normal range. I am happy with that.
My weight was down 78 kg (BMl 26.5), a percentage loss of over 16%, plus BP stable about 125/70.
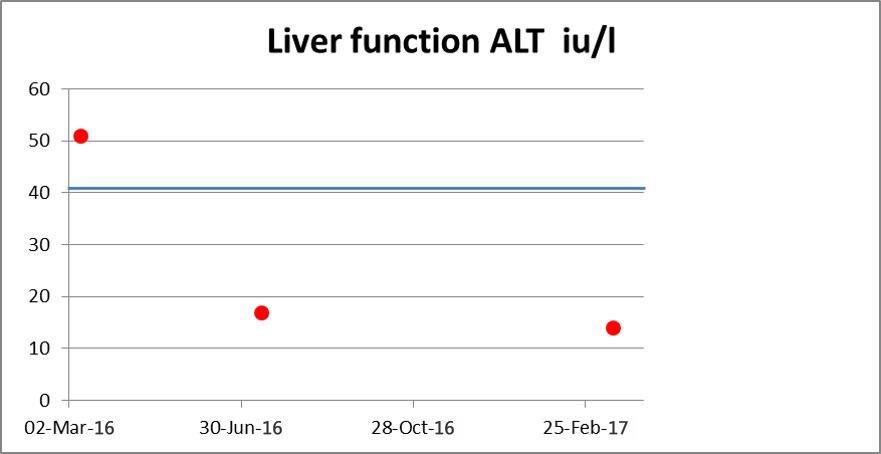
ALT liver function was also down from 52 to 18 iu/l, indicating a totally reversal of my fatty liver condition.
By November 2016 my weight was 70 kg (BMl 25.3), BP about 120/65 and HbA1c was 43 (6.0%).
I also have invested in a rowing equipment to supplement the walking.
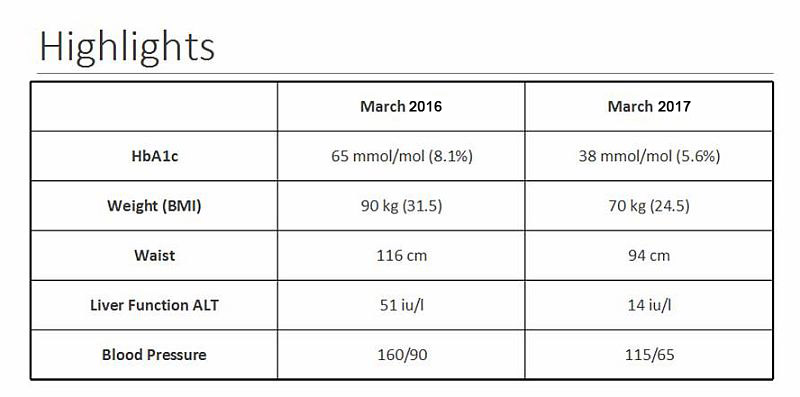
One year on, March 2017
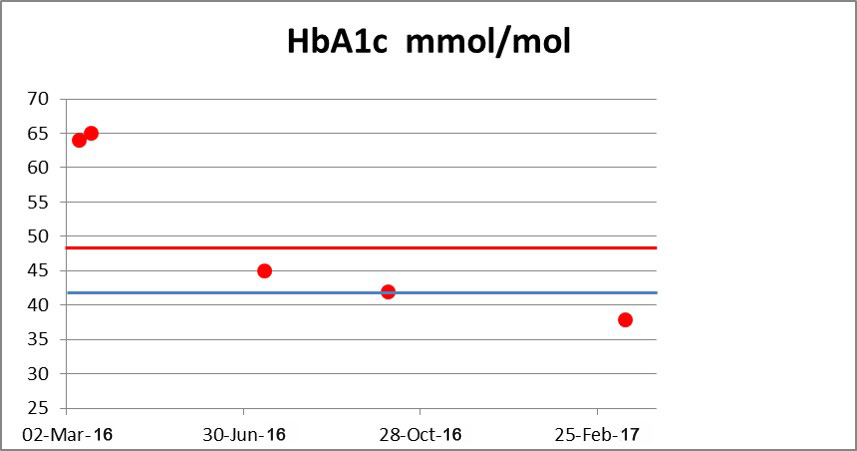
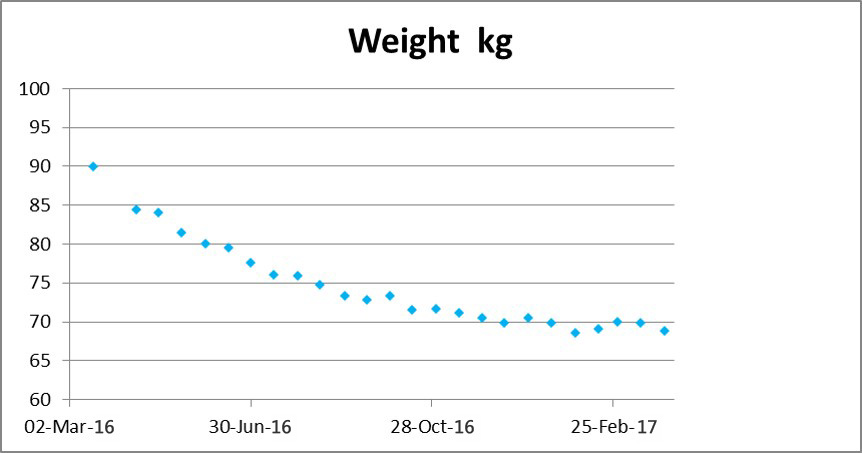
A picture speaks a thousand words, hence rather than more dull and lifeless text, and more graphs below covering the period from February 2016 to March 2017.
My HbA1c is 38 mmol/mol (5.6%) now which is surely within the non-diabetic range. Yet I am still a diabetic However I am protecting my remaining beta cell function in the pancreas as best as I can, plus avoiding exacerbating insulin resistance. It is all because of carbohydrate restriction, which also has reduced my triglycerides greatly, as well as the fat component of my LCHF diet has also helped increase my HDL-C to 1.95. So in this context the total cholesterol of 6.1 is definitely no concern to me. I feel very good.
The slight falls and rises in fasting blood sugar reflect life conditions like work stress – however at least through testing so I know what’s going on.
I am happy that my weight is stable at 70 +/- 1 kg (BMI 24.5) now, which represents a 20% loss in a year; and BP about 115/65. And my waist is 36 in (93cm) having been 50 in (118 cm) a year ago.
What do I eat now?
I have done all this without any medication, but just with exercise and diet. So what actually do I now eat with LCHF? Below is a typical meal each day:
Breakfast – cooked breakfast of tomato, mushrooms, eggs and bacon; and full fat Greek yoghurt with some berries occasionally. Coffee and/or tea with double cream.
Lunch –tapas style platter, select from olives, salami, a little hummus, cheese, guacamole, tomato, mackerel pate, salad leaves.
Dinner –a glass of red wine, double cream, berries, fish or meat with above-ground veggies or salad, avocado vinaigrette and double cream.
Snacks if needed–brazil nuts or cheese.
Decaffeinated tea or coffee and plenty of water after midday.
Selected reading
Max Sidorov – books 7 Steps to Health: What Pharmaceutical Companies Don’t Tell You About Diabetes, and Are Attempting to Cover up the Truth: The Truth About Low-Carb Diets; and the website www.myhealthlives.com/diabetes
Click Here to Watch the Diabetes Treatment Video of This Book Now
Thousands of people suffering from erratic blood sugar has been using this ground-breaking solution…
To help them burn away dangerous fat from their vital organs and bellies…
While stabilizing their blood sugar levels naturally and effectively.
And starting today…

Thanks for sharing, best diabetes book so far , recommended to me by my doctor. I love this book. I am a diabetic. This new way of eating does work. I am losing weight, removing toxins and the brain fog that contributes to my anxiety attacks is gone. My glucose numbers are regulating. This book is a God send!
Hi Lisa, I’m newly diagnosed type 2 & I have’nt a clue what I’m doing! I was given a blood testing kit & told to test it 4 times a day my lowest reading has been 9.2 my highest 27.0 not feeling very well & not that sure how to make myself better any ideas? Does this book really can help cure diabetes?
Charles,
My doctor recommended this book to me because another one of his patients followed the instructions and was able to stop taking all meds for diabetes, high blood pressure and chloresteral. Now, I’m using this book and follow the instructions to become free of diabetes. I have just started and i know the plan works so I’m looking forward to becoming healthy.
You can also give it a shot, I think it would works for you as me.
Lisa,
Thanks for your sharing, My blood sugar was getting to the pre-diabetic stage so I bought this book and followed the plan. I lost 15 pounds in six weeks. what was really interesting is that my blood sugar level dropped 14 points in the first week. I recommend this book to anyone worried about their blood sugar. It does work.
HI, I saw this on other websites and plan on purchasing it. When you started, did you stop your meds? Or did you use the same med dosages while using this method? Thank you
Hi, Cory,
I continued to use my metformin as prescribed. In about 3 – 4 months I reduced it by half…with my doctor’s approval. At the end of about 6 – 7 months I stopped taking it altogether. Also with my doctor’s approval. It’s now been almost two years and my blood sugar is normal. Although I test my blood sugar daily, my blood tests have been reduced from quarterly to bi-annual.
What is the name of the book that everybody keeps mentioning? Also where can I find it? Thank you
What is the name of the book , where can I buy it thanks